Challenges
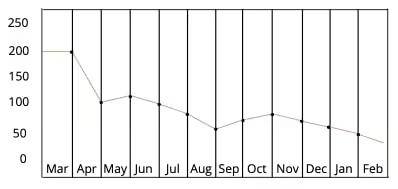
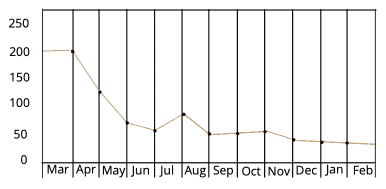
With 174 locations and more than 130 providers, one of the largest multi-specialty groups in the U.S. was struggling with an inability to scale, high staff turnover, missed re-enrollment dates, which ultimately contributed to cashflow disruptions.
“I have not found anything that compares to Med USA Provider Relations services. Your team always conveys control, confidence & competence."
Solutions
To address these challenges, the medical group partnered with Med USA for a provider relations solution that included payer enrollment, privileging services, licensure monitoring as well as ongoing maintenance and support for CAQH, PECOS, TMHP and PIMMS profiles.
Utilizing a time-tested, proprietary process and our highly trained team, Med USA helped this client successfully navigate the complicated maze of provider enrollment and credentialing - taking care of the details so the medical group could focus on taking care of their patients.