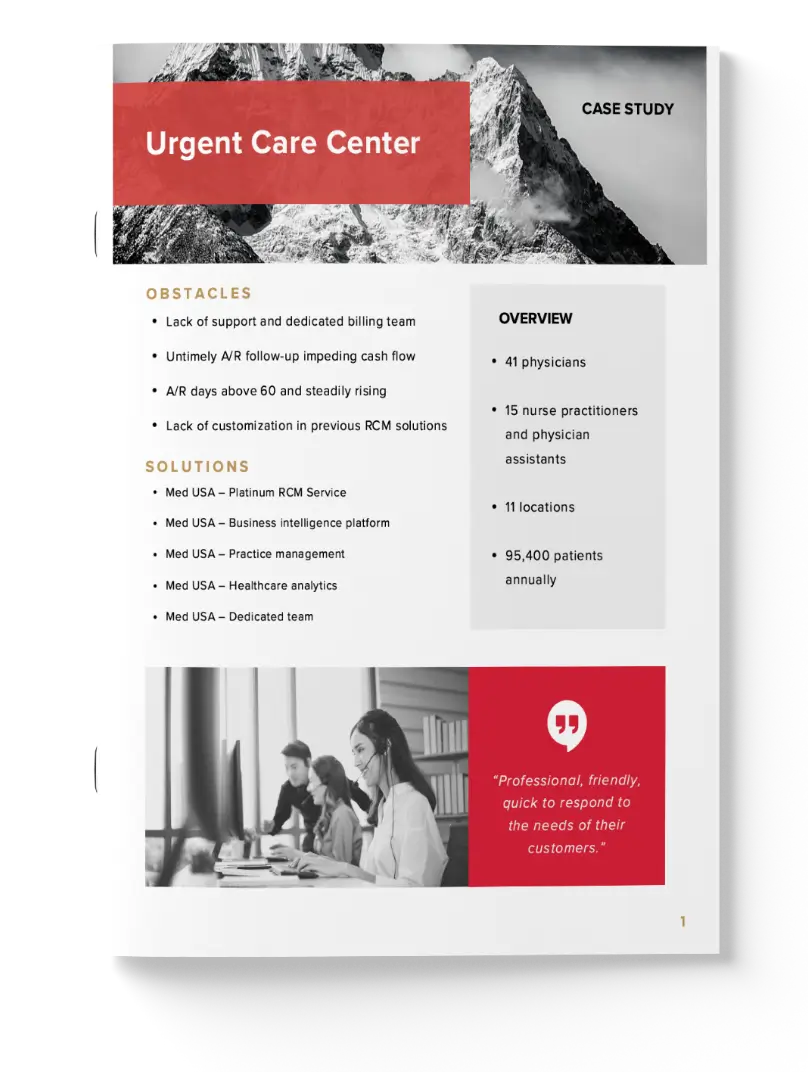
How an Urgent Care Center Increased Revenue per Visit by 25% With a 40% Decrease in A/R
When a large urgent care center lacked a dedicated billing team and urgent-care-specific revenue cycle workflows, they turned to Med USA to reduce climbing A/R, improve reimbursement consistency, and increase revenue per visit. Before partnering, the organization faced delayed charge capture, inconsistent eligibility verification, and limited visibility into denial drivers—issues that commonly inflate A/R days and suppress collections in high-volume urgent care settings. Med USA implemented urgent care–focused intake and charge workflows, payer-specific claim edits, and denial root-cause tracking to create measurable operational control. The result: a 25% increase in revenue per visit and a 40% decrease in A/R, driven by cleaner claims, faster follow-up, and fewer preventable denials. Download the case study to see the execution approach, KPIs tracked, and outcomes achieved.
Download the Case Study
Revenue Cycle Management
-
CHARGE POSTING
-
PATIENT CONTACT
-
INSURANCE REIMBURSEMENT
-
REAL-TIME ANALYTICS
-
REIMBURSEMENT & PAYER MANAGEMENT
Provider Relations
-
Credentialing & Enrollment
-
Provider re-credentialing
-
Contracting payer enrollment
-
Provider privileging
-
Expirable document management
On the Blog
Stay current on best practices for revenue cycle management, credentialing, and healthcare compliance